Myocarditis is an acute inflammatory condition that can have an infectious, toxic or autoimmune aetiology. Myocarditis can complicate many infections in which inflammation may be due directly to infection of the myocardium or the effects of circulating toxins. The clinical picture ranges from a symptomless disorder, sometimes recognised by the presence of an inappropriate tachycardia or abnormal ECG, to fulminant heart failure. Myocarditis may be heralded by an influenza-like illness. In most patients, the disease is self-limiting and the immediate prognosis is excellent. However, death may occur due to a ventricular arrhythmia or rapidly progressive heart failure. Myocarditis has been reported as a cause of sudden and unexpected death in young athletes. Some forms of myocarditis may lead to chronic low-grade myocarditis or dilated cardiomyopathy. The case report describes a case of parainfectious myocarditis in a 20-year-old patient.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
20-year-old patient without any internal diseases, with ongoing respiratory infection in ATB treatment on 2nd day, examined at the internal outpatient clinic for sudden chest pain at first on the left side of chest parasternally, later with propagation to the entire chest area. The patient reports a few days of persistent overall weakness, fatigue, fever up to 39.5 °C, productive cough, dyspnoea during physical activity. He did not collapse. Patient without cephalea and vertigo, with normal anovesical functions.
Physical examination: BP 114/79 mmHg TT 38,2 °C.
Patient conscious, oriented in place, time and person, active position, normostenic habitus, normal nourishment, skin without jaundice and cyanosis, eupnoic, without lateralisation. Pupils isocoric, bilateral fotoreaction, anicteric eyeballs, pink conjunctivas, orophyrynx reddened, tongue in a mid position, wet, uncovered, normal and symmetrical jugular vein filling, non-palpable lymphatic nodes and thyroid gland, symmetrically palpable pulsation of carotid arteries. Vesicular breathing, on the left side rales, regular heart rate, fr. 94/min., abdomen without pain and resistance during palpation, non-palpable liver and spleen, tapottement bilaterally negative, lower extremities without oedemas, pulsations on a. dorsalis pedis, a. tibialis posterior bilaterally palpable.
ECG: sinus rhythm, fr. 94/min., PQ 180 ms, QRS 90 ms, R/S V3-V4, ST without elevation/depression, T pozit., without ectopy.
Laboratory results:
CK 11,75 ukat/l*, CK-MB 0,68 ukat/l*, TnI 13,12 ug/l*, D-dimér 0,46 mg/l*, CRP 59,60 mg/l*, AST 1,54 ukat/l, GMT 2,53 ukat/l, PBNP 832,40 ng/l, the rest of lab. tests normal.
Differential diagnosis:
- Myocarditis
- Angina pectoris
- Acute myocardial infarction
- Pericarditis
- Aortic dissection
- Pulmonary embolism
- Tracheobronchitis
- Pneumonia
- Pneumothorax
- Gastro-oesophageal reflux disease
- Peptic ulcer disease
- Gallstones
- Pancreatitis
- Tietz´s syndrome
- Vertebrogenic algic syndrome of cervical spine
- Panic disorders (neurocirculatory asthenia)
Imaging methods:
Abdominal ultrasound: without a pathological finding on the organs of the abdominal cavity.
Echocardiography 1: Without dilatation of the heart cavities, left ventricle without regional kinetic disorders, no systolic dysfunction (EF LV 65%), without valvular disordes, no pulmonary hypertension, minimal pericardial effusion.
Chest X-ray: In the left lower lung field inhomogeneous shading, right pulmonary parenchyma without changes, diaphragm sharp, free angles, heart not enlarged.
Echocardiography 2 (after 4 days): Without dilatation of the heart cavities, diffuse left ventricular hypokinesis with mild to moderate systolic dysfunction (EF LV 40%), mitral and tricuspidal regurgitation in stage I, no pulmonary hypertension, no pericardial effusion.
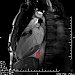
MR of the heart with contrast medium (Figure 1): Pathological subepicardial to intramural focus inferolaterally, character of fibrosis, probably inflammatory aetiology. Reduced EF LV 37%. Pneumonia l. sin. Smaller pericardial effusion. Fluidothorax bilat., praecip. l. sin.
24-hour ECG Holter: Constant sinus rhythm, with preserved circadian frequency variability, without supraventricular and ventricular extrasystoles, without supraventricular and ventricular tachycardia, with no asystolic pauses.
Diagnosis:
Myocarditis v. s. parainfectious Bronchopneumonia l. sin.
Therapy:
Viral infections are the most common causes, such as Coxsackie viruses B, influenza A and B viruses, CMV, EBV, HIV. Myocarditis may occur several weeks after the initial viral symptoms and susceptibility is increased by corticosteroid treatment, immunosuppression, radiation, previous myocardial damage and exercise. Some bacterial and protozoal infections may be complicated by myocarditis (diphtheria, Lyme disease). Toxic aetiologies include drugs, which may directly injure the myocardium (cocaine, lithium and anticancer drugs such as doxorubicin) or which may cause a hypersensitivity reaction and associated myocarditis (e.g. penicillins and sulphonamides), lead and carbon monoxide. Occasionally, autoimmune conditions such as systemic lupus erythematosus and rheumatoid arthritis are associated with myocarditis. Specific antimicrobial therapy may be used if a causative organism has been identified, however, this is rare and in most cases only supportive therapy is available. Treatment for cardiac failure or arrhythmias may be required and patients should be advised to avoid intense physical exertion because there is some evidence that this can induce potentially fatal ventricular arrhythmias.
In the case of our patient, empiric ATB treatment was initiated in double combination. Because of tachycardia, we started the treatment with beta blocker. Regular check-ups by cardiologist are required. In the prevention of myocarditis, it is advisable to have a rest and do not sport during the disease.
Authors declare the case report will not be published in any national or international publications.
Classification ICD-10:
I41.0 Myocarditis, J18.0 Bronchopneumonia
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Katarína Demková: Parainfectious myocarditis. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 17. 05. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=346. ISSN 1337-7000.