Kyphoscoliosis is a well-recognized cause of respiratory failure. Kyphoscoliosis is a chronic disease, occurring in 2-3% of the general population, which leads to a distorted spinal curvature and chest wall deformity. As a consequence, respiratory function is impaired due to reduced chest wall compliance and restrictive lung function pattern arises. The development of noninvasive ventilation (NIV) has made it an accepted standard modality of care at the present time for patients with chronic respiratory failure caused by kyphoscoliosis. The presented case report describes a 49-year-old female with idiopathic kyphoscoliosis who developed chronic hypercapnic respiratory failure with the need of noninvasive ventilatory support.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
49-year-old female was referred to Department of Pneumology and Phtiseology from 1st Department of Internal Medicine because of progression of dyspnoea and chronic hypercapnic respiratory failure. The patient had kyphoscoliosis from childhood without any recognized etiological factor, she did not undergo any kind of surgical intervention because of spine deformity, she was not seen by orthopedic physician regularly. One year prior to admission to our department she had been diagnosed with pulmonary embolism with acute respiratory failure and necessity of endotracheal intubation and invasive ventilation followed by short-term tracheostomy. She was regularly observed by cardiologist due to sinus tachycardia and by psychiatrist due to anxiety disorder. From her chronic medication she took warfarin as chronic anticoagulation therapy, beta blocker, antidepressives and statines. She was an ex-smoker, had stopped smoking 17 years ago, not married, worked as a consultant for estate agency.
Current disease: few days prior to hospital admission she noted slow progressive shortness of breath, she could not tolerate minimal physical activity. No chest pain, cough, fever or gastrointestinal problems occurred. Recurrent pulmonary embolism and acute coronary syndrome were excluded at internal department.
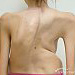
On physical examination, she was cyanotic (pulse oximetry saturation was 90%), tachycardic with regular heart frequency of 112 beats/minute, breathing was vesicular, without any side phenomena. The patient had severe kyphoscoliosis affecting the thoracic spine with a prominent hump.
Laboratory results:
Arterial blood gases showed severe chronic hypercapnic respiratory failure with a pH of 7,374, pCO2 of 8,11 kPa and pO2 of 4,55 kPa, which was compensated by retention of bicarbonates.
Imaging methods:
The chest X ray in posteroanterior projection showed severe deformity of thoracic spine with a removal of middle structures (Figure 1). No infiltrations were detected in visible part of lung parenchyma.
Pulmonary function tests proved severe restrictive ventilatory defect, forced vital capacity was decreased to 0,62 l (25% of predicted values).
Therapy:
In view of presented results of arterial blood gases, noninvasive ventilation via nasal mask with bilevel positive airway pressures delivering two different pressures between inhalation and exhalation creating the pressure support was started. We used the optional average volume assured pressure support mode that automatically adapts the inspiratory positive airway pressure to provide the preset patient´s tidal volume. Due to severe hypoxaemia, supplemental oxygen therapy was added to the ventilation circuit. The patient's tolerance of the treatment was good, during 17 days in hospital we found an improvement of patient´s clinical status and blood gases values. There was gradual decrease in daytime values of pCO2 and increase in daytime values of pO2. The NIV in combination with long-term supplemental oxygen therapy was recommended for chronic everyday use. The patient compliance to treatment has remained very good (average day usage 8 hours) throughout 3 years of follow-up with normalization of pCO2 levels (Figure 2). Patient´s quality of life has improved as well, she is still employed.
Diagnosis:
Chronic hypercapnic respiratory failure
Kyphoscoliosis
Discussion:
The respiratory system consists of two parts. The lung performs gas exchange and the pump ventilates the lung. The pump consists of the chest wall, including the respiratory muscles, and the respiratory controllers in the central nervous system (CNS) linked to respiratory muscles through spinal and peripheral nerves. When respiratory failure ensues, the respiratory system fails in one or both of its gas exchange functions - oxygenation of mixed venous blood and/or elimination of carbon dioxide (Figure 3).
The diagnose of respiratory failure is based on arterial blood gas assessment and it may present as acute, chronic or acute on chronic. Respiratory failure due to lung diseases (pneumonia, acute respiratory distress syndrome, cardiogenic pulmonary oedema, emphysema or interstitial lung disease) leads to hypoxaemia with normocapnia or even hypocapnia (type I respiratory failure = hypoxaemic respiratory failure). Failure of the pump results in alveolar hypoventilation and hypercapnia with parallel hypoxaemia (type II respiratory failure = hypercapnic respiratory failure). In some diseases, both conditions may coexist, hypoxaemia usually appearing first. Hypercapnic respiratory failure may be the result of CNS depression, functional or mechanical defects of the chest wall, an imbalance of energy demands and supplies of the respiratory muscles.
Kyphoscoliosis is a well-recognized cause of respiratory pump failure. The most common cause is idiopathic scoliosis which begins in childhood but it may occur also secondary to other disorders (Figure 4). Scoliosis (spinal curvature in the lateral plane) is usually associated with kyphosis (spinal curvature in the sagittal plane). In scoliosis, there is a relationship between the severity of the scoliosis as measured by the angle of the curvature in the spine (Cobb angle), and the risk of development of respiratory failure (Figure 5). The disorder affects the respiratory system due to decreased compliance of the chest wall. The stiff chest wall requires greater inspiratory effort for relatively small tidal breaths, which increases the work of breathing. However, respiratory muscle strength might be decreased because of intrinsic muscle weakness (as in secondary kyphoscoliosis due to neuromuscular disease) or because of the respiratory muscles act at a mechanically disadvantageous position because of the altered chest wall configuration. To prevent respiratory muscle fatigue patients adopt a pattern of rapid shallow breathing with a low tidal volume, leading to unequal ventilation of the lungs and pulmonary microatelectasis. Respiratory failure eventually develops once the output that can be generated by the respiratory muscles is insufficient to overcome the additional load placed on the system.
Once respiratory failure or cor pulmonale develops, life expectancy with conservative therapy is poor. Ventilatory support has been used in different forms in the treatment of patients with kyphoscoliosis and acute or chronic respiratory failure for the past 50 years.
Noninvasive ventilation is the application of respiratory support via a face-mask or helmet. NIV avoids intubation and its risks while preserving functions such as speaking and swallowing (picture 6). In the modern era it implies the application of positive airway pressure, however some classifications include the application of a negative-pressure generator to the chest (iron lung) as NIV, which was used in the past. Positive pressure ventilatory support may be with continuous positive airway pressure (CPAP) or bilevel positive airway pressure (BiPAP) modes and delivered by a range of ventilators from specifically designed devices to full-service ICU ventilators.
In patients with kyphoscoliosis NIV improves sleep architecture, and nocturnal and daytime arterial blood gases almost immediately after initiation. It might improve pulmonary mechanics, relieve work of breathing, as endurance time of the respiratory muscles may increase. Long-term usage of NIV has been reported to reduce hypoventilation related symptoms and dyspnea, improve mental function, reduce number of days spent in hospital and increase quality of life. Start of NIV in patients with kyphoscoliosis is indicated in combination of daytime hypercapnia and symptoms reflecting hypoventilation or the development of its associated complications. There is no evidence to start NIV “prophylactically” when patients at risk still have normal diurnal arterial gases. In many cases, ventilatory support via NIV may itself correct hypoxaemia, however in some patients supplemental oxygen is required as well. Survival in patient with chest wall disorders on long-term NIV is quite good, with a 5-year survival rate reported between 76% and 90%.
Authors declare the case report will not be published in any national or international publications.
Classification ICD-10:
J96.1 Chronic respiratory failure, M41.9 Scoliosis unspecified
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Ivana Trojová: Chronic Respiratory Failure due to Kyphoscoliosis. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 01. 05. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=315. ISSN 1337-7000.