Cardiac tamponade is a clinical syndrome caused by the accumulation of fluid or gas in the pericardial space, resulting in reduced ventricular filling and therefore decreased cardiac output (Figure 1). The condition is a medical emergency with resultant cardiogenic shock and death if not treated immediately. The presented case report describes a 63-year-old oncological patient who developed cardiac tamponade with the need of pericardiocentesis.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
63-year-old female was brought to internal emergency department of University Hospital in Kosice by ambulance because of chest pain and persisting hypotension. Verbal communication with patient was enabled because of tracheostomy.
Current disease: symptoms lasting for 2 days – chest pain, dyspnoea and faintness. The patient denied syncope, cough, febrilities, gastrointestinal or urogenital problems.
It was found out from patients´s documentation that she was diagnosed with laryngeal squamous cell carcinoma 3 years ago and underwent total laryngectomy and bilateral cervical discectomy with the need of tracheostomy. Postoperatively she was treated with radiotherapy and chemotherapy and was advised for regular follow-up on a routine outpatient basis which she ignored.
Initial vitals at emergency department revealed a blood pressure of 70/50...90/60...90/60 mmHg, pulse of 170...140...80 beats/minute. On physical examination she was eupnoeic, cachectic, jugular veins were not distended, tracheostomy present, lung sounds were clear bilaterally, heart sounds were not muted, lower limbs without a trace of edema.
The electrocardiogram (ECG) after quick parenteral rehydration in emergency room showed sinus rhythm of 80 beats/minute, low-voltages QRS complex amplitudes in limb leads, ST was isoelectric (Figure 2).
Laboratory assessment:
Laboratory investigation was significant for a mild decrease of white blood cell count and moderate normocytic normochromic anaemia. Liver function tests were elevated with mild hypoproteinemia and hypoalbuminemia. Cardiac and inflammatory markers were not elevated.
Imaging methods:
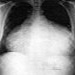
The chest X ray in posteroanterior projection on the day of admission showed enlarged cardiac silhouette (increased cardiothoracic ratio) without pulmonary congestion. Transthoracic echocardiography showed large pericardial effusion of about 500-600 ml with swinging motion of heart, left ventricle was normal in size and systolic function, left atrium, right atrium, and right ventricle were of normal size, mild pulmonary hypertension was detected. Examination also revealed presence of echo contrast masses which were suspicious to be cardiac metastases. One tumor (8x8 mm) was localized in right atrium, the other was behind left atrium (18x6 mm).
Therapy:
Because of clinical, radiological and echocardiographic picture suspicious of cardiac tamponade due to newly diagnosed cardiac metastases the patient was closely monitored with regular checks of vital signs and was parenterally rehydrated. Within a few days, an overall progression of clinical worsening was documented. The patients was severely dyspnoeic, hypotensive, with distention of jugular veins and decreased cardiac tones. Repeated ECG documented normal heart frequency but progression of low voltage of QRS complexes diffusely (Figure 3). Control echocardiography showed persisting swinging heart motion, large pericardial effusion of about 600-700ml with tamponade physiology, patient was indicated for pericardiocentesis and therefore referred to Department of Cardiology of East Slovak Institute of Cardiovascular Diseases.
Diagnosis:
Cardiac tamponade
Discussion:
Cardiac tamponade is caused by the buildup of pericardial fluid (exudate, transudate or blood) that can accumulate for several reasons. Hemorrhage, such as from a penetrating wound to the heart or ventricular wall rupture after an MI, can lead to a rapid increase in pericardial volume. Other risk factors, which tend to produce a slower growing effusion, include infection (TB, myocarditis), autoimmune diseases, neoplasms, uremia, and other inflammatory diseases (pericarditis). Pericardial fluid that builds up slowly is better tolerated in patients than rapid accumulations - hence traumatic causes (hemopericardium) require small volumes to causes hemodynamic instability versus pericardial effusions from medical causes such as malignancy where large volumes of fluid may accumulate in pericardial sac before patients become symptomatic.
Clinical signs in a patient with cardiac tamponade include tachycardia, hypotension, raised jugular venous pressure, muffled heart sounds. A key diagnostic finding is pulsus paradoxus (conventionally defined as an inspiratory decrease in systolic arterial pressure of 10 mmHg during normal breathing).
The diagnosis of cardiac tamponade can be suspected on history and physical exam findings. An ECG may show signs of pericarditis, with especially low QRS voltages and electrical alternans (Figure 4). Both ECG signs are generally considered to be an expression of the damping effect of pericardial fluid and swinging heart. Chest x-ray may show an enlarged heart (Figure 5) and may strongly suggest pericardial effusion if a prior chest radiograph with normal cardiac silhouette is available for comparison. Echocardiography is the single most useful diagnostic tool to identify pericardial effusion and estimate its size, location and degree of haemodynamic impact.
The treatment of cardiac tamponade involves drainage of the pericardial fluid, preferably by needle pericardiocentesis, with the use of echocardiographic or fluoroscopic guidance, and should be performed without delay in unstable patients. Alternatively, drainage is performed by a surgical approach, especially in some situations such as purulent pericarditis or in urgent situations with bleeding into the pericardium.
Authors declare the case report will not be published in any national or international publications.
Classification ICD-10:
4-D assessment:
Textbooks and manuals |
Educational websites and atlases |
Digital video |
Presentations and animations |
Casuistics in images |
E-learning courses (LMS) |
Unreviewed |
Undergraduate level |
Graduate |
Advanced Graduated |
Complex |
HodnoceníPlease select achieved education degree and then evaluate the teaching material particularly in light of material suitability for self-learning.
Student – student of bachelor or master degree
Graduate – graduate of bachelor or master degree PhD. Graduate – Ph.D. student, Ph.D. graduate, researcher, ...
%
Evaluate evaluatethis contribution first! |
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Ivana Trojová: Cardiac tamponade due to cardiac metastases. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 13. 03. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=310. ISSN 1337-7000.