Community-acquired pneumonia (CAP) is a serious public health concern and a major cause of mortality and morbidity. Despite advances in antimicrobial therapies, microbiological diagnostic tests and prevention measures, pneumonia remains the main cause of death from infectious disease in the world. An important reason for the increased global mortality is the impact of pneumonia on chronic diseases, along with the increasing age of the population and the virulence factors of the causative microorganism.
In 2013, the Global Burden of Disease Study based on data from 188 countries around the world, reported that lower respiratory tract infection was the second most common cause of death. In Europe, mortality rates for CAP vary widely from country to country, ranging from <1% to 48%.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
Current disease: 48-year old patient was referred to Department of respiratory diseases by general practitioner because of an X-ray finding of pneumonia localized in the inferior lobe of the right lung. She reported malaise, fever of 39.5°C with chills, worsened after paracetamol intake, subcostal pain on the right side, intolerance of right side position, shortness of breath while walking, mild cough with production of yellowish sputum and decreased appetite.
Personal history and medication: no previous chronic disease, no long-term medication
Habits: no smoking, no alcohol
Laboratory results:
Physical examination: normosthenic, body temperature 38°C, vesicular breathing, weakened on the right base of lungs, no side breathing noises, abdomen sensitive of under right rib cage
Inflammatory markers: CRP 144.63 ml/L, PCT 4.580 ug/L
Other laboratory findings: Alb 34.6 g/L, Total proteins 58.4 g/L, K 3.0 mmol/L
Hemogram: Hgb 9.28 g/dL, RBC 3.72 x109 /L, HCT 0.28, MCV 74.74 fL, MCH 24.9 pg - microcytic anemia
WBC 13.20x109 /L, Neu abs 11.89 x109 /L, Ly abs 0.59 x109 /L, Neu 90.1%, Ly 4.45% - leucocytosis with neutrophilia
Serology: in urine positivity of Streptococcus pneumoniae antigen, in serum Candida manan antigen positivity
We did not verified an invasive candida, but with positive Candida-mannan antigen in serum, antibiotic treatment combined with antimycotic to cover the entire proven flora, keeping it in the treatment within 7 days. Serology for chlamydia and mycoplasma was also performed, the result was negative.
Imaging methods:
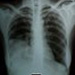
Chest X-ray:
- Posteroanterior on admission: large, diffusely homogenous merging infiltrates in lower and partially middle right pulmonary lobe, cranially limited by horizontal fissure, right diaphragm and costophrenic angle indistinguishable (Figure 1)
- Posteroanterior on follow-up – 8 days later: partial regression of infiltration shadow, unveiling streaky shadow in the whole width of hemithorax, right diaphragm covered by homogenous cranially pulled shadow, probably of pleural origin (Figure 2)
- Left lateral on follow-up – 8 days later: shadow of pleural origin filling anterior angle, from where the shadow is pulled cranially and dorsally toward hilus, its width ranging from 4 to 2.5 cm, and reaching supraphrenically in width 3.5 cm to several mm in posterior angle (Figure 3)
Therapy:
ceftriaxon, ciprofloxacine, fluconazol, metamizol, nadroparine, potassium chloride, rehabilitation
Laboraty findings after therapy:
Inflammatory markers: CRP 23.85 ml/L
Hemogram: WBC 6.12x109 /L, Neu abs 3.55 x109 /L, Ly abs 1.59 x109 /L, Neu 58.1%, Ly 26.05%
Diagnosis:
Pleuropneumonia lateris dextri
Moderate microcytic anemia
Hypokaliemia
Hypoproteinemia
Discussion:
Pneumonia infection is the result of a complex process where the lower respiratory tract suffers the invasion of an infective microorganism. Pneumonia can be acquired in the community or acquired in the hospital environment, and can be transmitted by the aspiration of a pathogenic microorganism or by inhalation of a pathogenic microorganism.
Common respiratory symptoms of pneumonia include cough, often with sputum production or haemoptysis, dyspnoea, and pleuritic pain, non-respiratory symptoms like fever, myalgia, joint pains and herpes are also frequent.
Assessment of severity is crucial for decision whether treatment is conducted in outpatient setting or in hospital ward. Radiographic findings, comorbidities and physical examination findings should be considered. Several scoring systems were developed in order to aid the judgment such as PSI (pneumonia severity index) or CURB-65 (Figure 4 and 5).
Although microbiological diagnosis of CAP is fundamental to ensure appropriate antibiotic therapy, microbial diagnosis of pneumonia is achieved in less than 50% of cases and antimicrobial therapy should be empirically administered in order to avoid the delay in establishing appropriate therapy, associated with significant mortality.
Microbiological diagnosis of CAP continues to be based on respiratory samples or blood culture. The main problems with these conventional methods are the low yield and long turnaround time (48–72 h) and the fact that previous antibiotic use affects microbiological results. According to CAP guidelines, an optional microbiological diagnostic test in low to mild cases of CAP is recommended and in special situations it should be preferred. In the case of severe CAP it is recommended to take blood cultures, sputum staining, sputum culture, and the urinary antigen test for Legionella and Streptococcus pneumoniae.
Globally, Streptococcus pneumoniae (pneumococcus) is the most common pathogen causing community-acquired pneumonia, usually presented with acute symptoms of lower respiratory tract infection, historically called “typical presentation”. Pneumococcus was considered one of the 9 bacteria of international concern in the recent worldwide report of global antibiotic resistance published by the World Health Organization (WHO) in 2014.
Estimated prevalence of 19.3% to 34% was reported for S. pneumoniae in Europe. The diagnosis of pneumococcal pneumonia has increased significantly in recent years, mainly due to the introduction of the pneumococcal urine antigen test (routinely available from 2000 in most countries).
Performing blood cultures in patients before a previous antimicrobial treatment has a high specificity but a low positivity (less than 20% of the cases). Sputum sample collection is performed before patients initiate antimicrobial therapy (Figure 6).
Treatment for pneumonia includes antimicrobial therapy, supportive therapy, oxygen, and sometimes mechanical ventilation.
Patient presented in this case suffered from pneumonia with pleural reaction. Her general practitioner referred her to hospital because infiltration on chest X-ray included more than one pulmonary field. There was positivity of streptococcal antigen in urine, thus she was treated with antibiotics (cephalosporin and fluoroquinolone combined) and antimycotic therapy due to positivity of Candida antigen. Only partial resolution was visible on radiograph after 8 days of treatment but clinical status and laboratory findings were drastically improved. Total duration of antibiotic therapy was 14 days with recommendation of follow-up X-ray after the therapy.
Authors declare the case report will not be published in any national or international publications.
Classification ICD-10:
| Link | Date | Availability [?] | Clinically sensitive [?] | Licence | |
|---|---|---|---|---|---|
| National Center for Biotechnology Information | 1.1.2018 | anyone | – |  |
4-D assessment:
Textbooks and manuals |
Educational websites and atlases |
Digital video |
Presentations and animations |
Casuistics in images |
E-learning courses (LMS) |
Unreviewed |
Undergraduate level |
Graduate |
Advanced Graduated |
Complex |
HodnoceníPlease select achieved education degree and then evaluate the teaching material particularly in light of material suitability for self-learning.
Student – student of bachelor or master degree
Graduate – graduate of bachelor or master degree PhD. Graduate – Ph.D. student, Ph.D. graduate, researcher, ...
%
Evaluate evaluatethis contribution first! |
Courses
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Ivana Paraničová: Pleuropneumonia. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 21. 02. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=343. ISSN 1337-7000.