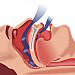
Obstructive sleep apnoea (OSA) is characterized by repetitive episodes of interruption of breathing during sleep due to partial or complete collapse of pharynx. Prevalence of mild OSA is about 9-24%, clinically significant disease is present in about 4% men and 2% women. Morphology of upper airways and body weight are important factors for development of OSA. Approximately 70% of OSA patients are overweight and 40% obese patients suffer from OSA.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
Sleep anamnesis: 41-year old patient was referred by otorinologist to Sleep-related breathing disorders out-patient clinic. He reported snoring for 30 years with observed apnoeic pauses during the last 2 years. His sleep routine was regular, sleep duration 8-8.5 hours, sleep latency very short. Nocturnal awakenings 3-5 times per night, because of urination and choking, dry mouth and profuse sweating. Loud snoring, in every position, patient awoke of his own snoring. In the morning he felt unrefreshed, he reported headaches, dry mouth, daytime sleepiness, involuntarily falling asleep while engaged in monotone activities, he often took a nap for 1 hour during the day. He denied any cognitive difficulties. He conveyed leg swelling and cough while in supine position. 10 years ago he gained 40 kilograms of weight.
Personal history: arterial hypertension, crural varices, lower back pain
Medication: lisinopril, amilorid, hydrochlorotiazide, diclofenac
Habits: ex-smoker for 10 years, smoked for 20 years about 40 cigarettes a day
Patient was admitted to hospital in order to diagnose sleep-related breathing disorder and setup of treatment.
Laboratory results:
Anthropometry: Height 175 cm Weight 170 kg BMI: 55.51 kg/m2
Physical examination: hyperstenic, exogenous obesity, eupnoea, oropharyngeal patency Mallampati grade 4, varices of lower limbs and chronic trophic skin changes
Blood gases:
- Saturation by pulse oximetry: 93%
- Arterial blood gases: pH 7.430 pCO2 5.94 kPa pO2 8.01 kPa, SaO2 92.0%, cHCO3 29.10 mmol/L – mild hypoxaemia, with no hypercapnia, with bicarbonates retention suggestive for night-time hypoventilation
Spirometry and body plethysmography: no ventilatory impairment, mild decrease of FVC, TLC on lower limit (Figure 1)
Epworth sleepiness scale: 12 points - a questionnaire for evaluation of daytime sleepiness (Figure 2) - 10 and more points indicate severe daytime sleepiness
Imaging methods:
Chest X-ray: no infiltration in parenchyma, accentuated hilar shadows (Figure 3)
Polysomnography: severe obstructive sleep apnoea of apnoeic-hypopnoeic index 113.1 episodes/h, with severe desaturations of average saturation in REM sleep 75% and 82% in NREM sleep, with desaturation index 105 episodes/h, time in saturation below 90% was 374 min, with hypoventilation in 28.8% of sleep, with disrupted sleep with reduction of slow wave sleep and REM sleep, with snoring (29.1% of sleep duration). Dominant type of respiratory episodes was mixed apnoeic episodes that start as central due to absence of respiratory centre activity and continue as obstructive (Figure 4 and 5).
Therapy:
Patient was treated with continuous positive airway pressure with oronasal mask (Figure 6). Effective therapeutic pressure was 18 cmH2O. At this pressure we attained reduction of apnoeic-hypopnoeic index from 113.1 to 6.4 episodes/h. (Figure 7), reduction of desaturation index from 105 to 5.1 episodes/h, increase of average saturation from 75% in REM and 82% in NREM to 95.5%, reduction of time under 90% saturation from 374 min to 54 s (Figure 8).
In arterial blood gases we observed increase of pO2 from 8.01 to 9.87 kPa, decrease of pCO2 from 5.94 to 5.37 kPa, decrease of bicarbonates from 29.10 to 25.80 mmol/L and increase of saturation from 92% to 95.8%.
Subjectively patient reported being completely refreshed after night sleep, he denied any breathlessness.
Diagnosis:
Severe obstructive sleep apnoea
Conclusion:
Follow-up: After 7 months of using CPAP patient was examined. Compliance of CPAP use was 5 hours per night, residual apnoeic-hypopnoeic index was 2.9 episodes/h. Patient was feeling incomparably better in terms of reduction of daytime sleepiness, he lost weight but he was unable to tell how many kilograms.
Discussion:
Sleep apnoea refers to repetitive episodes of cessation of air flow during sleep for at least 10 seconds; hypopnoea is an episode of flattened breathing followed by desaturation and/or arousal. Indicator of sleep apnoea severity is the apnoeic-hypopnoeic index (AHI), i. e. number of episodes per hour. The majority of respiratory episodes are obstructive in which partial or complete collapse of pharynx occurs due to a loss of muscle tone during sleep. Respiratory effort is still present. In central sleep apnoea loss of airflow is a result of respiratory centre inactivity, thoracic and abdominal movements are not present. In mixed sleep apnoea the episode starts as central apnoea and continues as obstructive.
An episode of obstructive apnoea or hypopnoea leads to an increase of inspiratory effort, deepening of negative intrathoracic pressure, acute hypoxaemia and hypercapnia. These changes activate sympathetic nervous system and together with brain cortex result in an arousal from sleep. In arousal, muscle tone in pharynx rises, airways reopen with short compensatory hyperventilation, blood gases are normalized, and one can hear explosive snoring sounds (Figure 4).
In frequent cyclic repetition of these changes, chronic intermittent hypoxia, sustained sympathicotonia and sleep fragmentation develop. These chronic consequences cause typical symptoms and complications (Figures 9 and 10).
Obesity, mainly central obesity, contributes to OSA mainly by peripharyngeal deposition of fat tissue, possibly by infiltration of submucosa by fat cells. Obesity reduces functional residual capacity and caudal traction on upper airway structures from mediastinal, rib cage and cervical strap muscle attachments which substantially increase pharyngeal collapsibility.
This patient was diagnosed with severe obstructive sleep apnoea and his subjective symptoms and objective findings were consistent with literary data. Patient was treated with continuous positive airway pressure with excellent objective and subjective effect. Furthermore, weight loss is inevitable part of treatment plan for such patient.
Authors declare the case report will not be published in any national or international publications.
Classification ICD-10:
E66.02 Obesity with BMI: 40 and more, G47.31 Obstructive sleep apnoea
Courses
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Ivana Paraničová: Obstructive sleep apnoea in extremely obese patient. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 03. 06. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=323. ISSN 1337-7000.