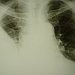
Case report presents patient with thoracic empyema, who was admitted in hospital after failure of outpatient antibiotic treatment. Patient suffered from fever, thoracic pain, dyspnea and dry cough. Chest X-ray revealed homogenous shadow in right basal and middle lung zone which was confirmed by CT. According to CT scan we expected presence of empyema. Patient was treated with combination of intravenous antibiotics and pleural puncture was performed. Analysis of sample showed results which met the criteria for empyema and patient was immediately sent to department of thoracic surgery for drainage.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
63 year old patient treated only for hypertension was admitted to Department of respiratory medicine and tuberculosis. Reason for admition was pleural effusion in right hemithorax. Patient was active smoker with 40 years smoking history. He smoked 20 cigarets per day and we calculated 40 packyears of smoking. He denied drinking alcohol and drank 3 cups of coffee daily. He was regularly observed by nephrologist due to incidental finding of renal cysts, several years ago he underwent cholcystectomy and last year polypectomy of colon. He was retired, in past he worked as a driver in concrete plant. In current disease, 10 days before admition he started to be subfebrile and febrilities over 38 degrees centigrade regularly occured in the evenings. Few days ago he started to complain about pain in back and on the right hemithorax and progressive dyspnea. Pain was provoked by cough, deep inspiration and change of position and last night disturbed his sleep. Cough was mostly non productive. He also lost appetite for 1 week. 3 days before admition his general practitioner prescribed him a broad spectrum antibiotics amoxycilin- clavulanic acid.
Physical examination:
Patient was eupnoic, afebrile, acyanotic in addmition. pulsoximetry revealed mild hypoxemia (oxygen saturation - SPO2: 87 % ). Within auscultation we observed alveolar breathing wihout side phenomena, but breathing was diminished in two-thirds on right side of thorax. Precussion was dulled on right side in descripted area. Physical finding on abdominal region and lower limbs was normal.
Laboratory assessment:
Haematolocical screening showed mild normocytic normochromic anaemia, expressive leucocytosis with neutrophylia (Table 1). Biochemical analysis documented elevation of inflammatory markers (C- reactive protein- CRP 287 mg/l), mild hypoproteinaemia with hypoalbuminaemia, hypochloraemia and retention of urea and creatinine (Table 1).
Imaging methods:
Chest X ray documented sharply bounded shadow over the basal and middle zones of right lung due to circumferential pleural thickening which lead to right lung volume loss. Visible parenchyme was obviously not affected. Left hilus was not enlarged, right was not evaluable, it was covered by shadow. Right diaphragm was not evaluable neither the phrenic angles. Heart shadow was apparently shifted to the left. Mediastinum was was not evaluable due to rotation.
Chest CT scan: Finding: CT scan documents lung parenchyme condensation with air-bronchogram in right lower lung lobe - a combination of inflamed tissue and parenchyme atelectasis due to thoracic empyema. Condensation was present also in right upper and middle lung lobe and was of subpleural localisation. Tracheobronchial tree was free without patologic contents, left leural space and percardium was without patologic contents. Contrast examination documented liquid-gaseous collection in right pleural space (see appendix CT scan- marked with arrow) and also in interpleural space with enhanced pleura. Pleura was thickened (width up to 4.3 cm) with obvious septations. Mediastinum was obviously shifted to the right, heart shadow had normal size. Secondary finding was presence of intrapulmonary and mediastinal lymphadenomegaly (possible reactive enlargement of lymphatic nodes) with size up to 2 cm. Lung hili were normally configured.
Diagnosis:
Thoracic empyema (pyothorax)
Differential diagnosis:
Tuberculous pleuritis
Malignant pleural effusion
Treatment:
Combined antibiotic therapy was administered immediately and combination of III.rd generation cephalosporin (Ceftriaxon) and chinolone (Ciprofloxacin) was used. Antibiotics were administered intravenously. Besides that patient received antipyretic drugs, regulated oxygenotherapy (due to desaturation) and nutritional support. Pleural puncture in right posterior axillary line was performed and sample of pleural effusion (which was turbid and yellow) was sent to laboratory. Therapeutic evacuation of effusion was not successfull due to high density of fluid. Biochemical analysis (table 2) on the basis of Light´s criteria (see table 3- division of pleural punctates) revealed presence of exudate with increased proportion of proteins and albumin. Considering high amount of lactatedehydrogenase (LDH- 120 ukat/l), low level of glucose (0.4 mmol/l) and low pH (7.12) we diagnosed empyema. This finding was not longer suitabe for conservative treatment and surgical therapy was indicated. Patients was transfered to department of thoracic surgery, where he underwent thoracotomy, decortication, plural space lavage and drainage. After removal of drain on 4th day, patient was discharged. with recommendation of rehabilitation.
Discussion:
In times of broadly used antibiotics is thoracic empyema rare but still occuring infectious disease. In clinical practice if symptoms are present it is important to perform chest x-ray in two projections. In case of confirmation of diagnosis of pleural effusion the next step is pleural puncture. Antibiotic therapy in combination is necessary and in case of complicated parapneumonic effusion or empyema surgical treatment is indicated.
Authors declare the case report will not be published in any national or international publications.
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Pavol Pobeha: Thoracic empyema. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 17. 05. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=306. ISSN 1337-7000.