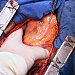
The case report describes the hospitalization of a 58 year old male admitted to our department for documented ischemic heart disease with affection of three coronary arteries. The patient underwent a cardiac surgery with the formation of one bypass with arterial graft and one bypass with venous graft. In the postoperative period, fibrillation of atrial fibrillation with successful cardioversion was noted. The patient was admitted to outpatient care on the seventh postoperative day.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
58-year-old man
PA: Diabetes mellitus (treated for 25 years), hypoglycaemic coma in anamnesis, surgery of haemorrhoids, gastroesophageal reflux, hyperlipidaemia treated by statins, VAS, anxiously depressive syndrome
FA: sister - treated diabetes mellitus
PA: Insulin (Novorapid 11-6-6j; Trosiba 20j – 21:00), Talliton 25mg (1/2-0-1/2), Prenessa 2mg (1-0-0), Preventax 100mg (0-1-0), Enelbin (1-0-1), Noflux 10mg (1-0-0), Atorvastatin 40mg (0-0-1), Dobica (1-0-1)
AA: penicilin (exanthema)
DA: ex-smoker (12-50-years-old)
SA: retired, living with his wife
AD: The patient reported a palpitation with spontaneous withdrawal and pressure chest pain during exercise. Due to the symptomatology and cummulation of risk factors for coronary artery disease (IHS), ambulatory cardiologist has performed ergometry. The result of stress ergometry showed signs of silent ischemia. Patient admitted to
cardiology for coronary examination.
Laboratoty results:
ECG: SR, 80min-1, EOS: intermed., PQ 160ms, QRS 100ms, QT: 300ms, STD desc. up to 3mm with negat. T in pre-cardiac electrodes, STD up to 1,5mm v I, II, III, aVF, without ectopia
Lab.: normal values
Imaging methods:
ECHO: Aortosclerosis. Dilatated aortic bulb (41 mm), left ventricle of normal size, no hypertrophy, no segmental kinetic disorders, LVEF: 60-65%, diastolic dysfunction - grade I, left atrium (43mm), mitral insufficiency – grade I, tricuspid insufficiency - grade I, no signs of pulmonary hypertension, no pericardial effusion.
SCG: Common left coronary artery: distal 60% stenosis, RIA: proximal bifurcation stenosis (RIA / RD1) 70-80%, median 1-1-1 and at the beginning of the middle part 90% stenosis; RD1: 70% at beginning, RCX: 50% to 60% stenosis, proximal stenosis 60%, middle bifurcation stenosis (RCX / RM1) 80%, median 1-1-1; ACD: sclerotic section with stenosis up to 80% in the middle part; The RPLD has a stenosis at the end of the middle part about 90%.
Diagnosis:
IHD, stable AP, 3-coronary artery disability, normal LVEF
Arterial hypertension 2nd. degree ESH/ESC VKVR
Diabetes mellitus I with chronic complications
Gastroesophageal reflux
Dyslipidaemia treated by statins
Chronic polytope VAS
Anxiously depressive syndrome
Ex-smoker
Therapy and conclusion:
Treatment strategy:
Patient transferred to a heart surgery department for surgical revascularization (CABG).
Surgery:
CABG in ECC, LIMA to RIA, VSM to RM1, (ACD and RIP nonrevascularizable because of atherosclerotic changes and insufficient vessel diameter) – CPB time: 43min, aortic clamping time: 23min.
Postoperative course:
The postoperative course complicated by the atrial fibrillation onset. Pharmacological conversion was ineffective. Electrocardioversion was performed and SR was induced. On the 7th postoperative day released to outpatient care.
Abbreviations:
ACD – right coronary artery; AP – angina pectoris; CABG – aortocoronary bypass; CPB – cardiopulmonary bypass; ECHO – echocardiography; IHD – ischemic heart disease; LCA – left coronary artery; LIMA – left internal mammalian artery; LVEF – left ventricle ejection fraction; RCX – ramus circumflexus; RD1 – firs diagonal branch; RIA – left anterior descending artery; RIP – ramus interventricularis posterior; RM1 – first marginal branch; RPLD – ramus posterolateralis; SCG - coronarography; SR – sinus rhythm; STD – ST segment depression; VAS – vertebral pain syndrome; VSM – great saphenous vein
Authors declare the case report will not be published in any national or international publications.
4-D assessment:
Textbooks and manuals |
Educational websites and atlases |
Digital video |
Presentations and animations |
Casuistics in images |
E-learning courses (LMS) |
Unreviewed |
Undergraduate level |
Graduate |
Advanced Graduated |
Complex |
HodnoceníPlease select achieved education degree and then evaluate the teaching material particularly in light of material suitability for self-learning.
Student – student of bachelor or master degree
Graduate – graduate of bachelor or master degree PhD. Graduate – Ph.D. student, Ph.D. graduate, researcher, ...
%
Evaluate evaluatethis contribution first! |
Courses
- Clerkship - Surgery [ChK/OPCH-V/16]
- Surgery [ChK/CH-SS-V/17]
- Surgery [1.ChK/CH-SS-ZL/16]
- Surgical Propedeutics [ChK/CHP-V/15]
- Surgery 1 [ChK/CH-V1/16]
- Surgery 1 [ChK/CH-ZL1/16]
- Surgery 2 [ChK/CH-V2/09]
- Surgery 2 [ChK/CH-ZL2/15]
- Surgery 3 [ChK/CH-V3/17]
- Surgery 3 [ChK/CH-ZL3/15]
- Surgery 4 [ChK/CH-ZL4/15]
- Surgery 5 [ChK/CH-ZL5/15]
- Surgery 6 [ChK/CH-V6/15]
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Tomáš Toporcer: Aortocoronary bypass. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 08. 05. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=300. ISSN 1337-7000.