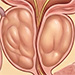
This article describes the Benign Prostatic Hyperplasia (BPH) that is the non-malignant adenomatous overgrowth of the periurethral prostate gland, specifically involving the transition zone. It is one of the most common conditions in aging men, with a histological prevalence reaching approximately 90% by age 85.
1. Pathophysiology Hyperplasia vs. Hypertrophy: Despite the name "hypertrophy" sometimes being used, it is truly a hyperplastic process involving an increase in the number of stromal and epithelial cells. Hormonal Influence: Development is androgen-dependent. Testosterone is converted to dihydrotestosterone (DHT) by the enzyme 5-alpha-reductase (primarily Type 2 in the prostate). DHT binds to androgen receptors, stimulating growth factors that lead to cellular proliferation and inhibited apoptosis. Mechanical Obstruction: Enlargement of the transition zone compresses the prostatic urethra, increasing resistance to urinary outflow.
2. Clinical Presentation (LUTS) Symptoms are collectively known as Lower Urinary Tract Symptoms (LUTS) and are divided into two categories: Obstructive (Voiding): Hesitancy, weak stream, intermittency, straining to void, and terminal dribbling. Irritative (Storage): Frequency, urgency, and nocturia.
3. Diagnosis Digital Rectal Examination (DRE): Used to assess size, contour, and consistency. A BPH-affected prostate typically feels smooth, firm, and elastic. International Prostate Symptom Score (IPSS): A validated questionnaire to quantify the severity of symptoms. Urinalysis & PSA: Performed to rule out urinary tract infections (UTIs) or prostate cancer. Uroflowmetry/Post-Void Residual (PVR): Measures the rate of urine flow and the amount of urine remaining in the bladder after voiding.
4. Management Watchful Waiting: Appropriate for mild symptoms (IPSS < 8). Pharmacotherapy: Alpha-blockers (e.g., Tamsulosin): Relax smooth muscle in the bladder neck and prostate to provide rapid symptom relief. 5-alpha-reductase inhibitors (e.g., Finasteride): Block the conversion of testosterone to DHT, physically shrinking the prostate over 6–12 months. Surgical Intervention: Reserved for severe symptoms or complications (e.g., refractory retention, bladder stones, recurrent UTIs). The "gold standard" is Transurethral Resection of the Prostate (TURP)
There are 4 anatomic zones of the prostate (anterior, peripheral, central and transition zone). In most cases BPH develops in the transition zone. BPH is proliferation of the epithelial and smooth muscle cells. Hyperplastic tissue leads to narrowing of the prostatic urethra and subsequent bladder outlet obstruction. Lower urinary tract symptoms include obstructive symptoms (decreased urinary stream, hesitancy, straining, incomplete bladder emptying) and irritative symptoms (urinary frequency, urgency, nycturia) as a result of hypertrophic detrusor muscle. Incidence of BPH is high, nearly 80 % of men will develop BPH and 30 % will receive treatment.
Diagnostics
Detailed history of voiding problems with the use of International prostate symptom score (IPSS) questionnaire can help in diagnosis. Important in diagnosis is physical examination (especially digital rectal examination of the prostate), laboratory examination - urinalysis, blood level of prostatic specific antigen (PSA) and creatinin. Objective parameter for treatment decision can provide uroflowmetry (urinary flow rate < 15 ml/s is clinically significant), transabdominal or transrectal ultrasonography (volume of the prostate ≥ 30 ccm is clinically significant) and determination of post-void residual urine volume (≥ 50 ml resp. ≥ 200 ml clinically significant resp. very significant) (9,10).
Management
Watchfull waiting is preffered in patients with mild symptoms. Farmacologic therapy could be used in patients with moderate to severe symptoms. Most often are used: - alpha-1-adrenergic receptor blockers (alpha blockers): tamsulosin, terazosin, doxazosin, alfuzosin, silodosin improve symptoms of BPH - 5-alpha-reductase inhibitors: finasteride or dutasteride help to shrink the prostate volume by decreasing the production of dihydrotestosterone in acinar glands of the prostate - phospodiesterase-5 inhibitors: tadalafil is efficacious in improving LUTS and concomitant erectile dysfunction. Surgical treatment is preffered method of treatment in patients with complications of BPH (urinary retention, recurrent urinary tract infections, recurrent gross hematuria, bladder stones and renal insufficiency due to subvesical obstruction). Transurethral incision of the prostate (TUIP) is used in small (< 30 ccm) obstructive prostate. Transurethral resection of the prostate (TURP) is „gold standard“ treatment. Resectoscope is inserted through urethra in prostatic urethra and during continual fluid irrigation prostatic tissue is resected with an electrical loop and pieces of tissue are flushed out at the end of the procedure. Open simple prostatectomy is used if the prostate is too large (more than 80 ccm). Laser surgical procedures include Photoselective vaporisation of the prostate (PVP - laser energy destroys the prostate tissue), Holmium laser enucleation of the prostate (HoLEP) or Thulium laser enucleation of the prostate (ThuLEP). The last two can be used also for large BPH without risk of high blood loss. There are some adverse effect of surgical treatment. Sometimes it is bleeding, which is less common in laser procedures. Also absorption of irrigation fluid during prolonged procedure can cause TUR syndrome (fluid overload and dilutional hyponatremia) which is less commonly in bipolar TURP. Retrograde ejaculation is very comon. Damage of urinary sphincter may result in urinary incontinence and damage to pudendal nerves may cause erectile dysfunction. Minimally invasive therapy can be used in patients with high risk for general anesthesia: prostatic urethral lift, water vapor thermal therapy and high-intensity focused ultrasound (HIFU).
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Keywords: Benign prostatic hyperplasia. transurethral resection, lower urinary tract symptoms, obstructive symptoms, nycturia
citation: Ľubomír Lachváč: Benign prostatic hyperplasia. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 29. 04. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=676. ISSN 1337-7000.