Appendicitis is one of the most common reasons for surgery and emergency hospitalization due to acute abdominal pain. Accurate diagnosis of acute appendicitis and subsequent indication for surgery can prevent complications. Conversely, the surgeon´s decision to operate with the aim of avoiding the complications of a late surgical intervention in positive appendicitis cases leads to negative appendectomy in 10,5% of the cases.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
Anamnesis:
A 23-year-old man presented with a two days history of abdominal pain that started as epigastric pain and became located in the right lower quadrant. He also experienced loss of appetite, nausea and vomiting.
He had undergone no previous abdominal or pelvic surgery.
Examination and laboratory results:
His physical examination revealed tenderness in the right iliac fossa, local guarding and rebound tenderness at the McBurney point, without psoas or obturator sign. Abdominal examination revealed two positive signs consistent with signs of acute appendicitis: Plenies´s and Blumberg´s sign. Rowsing´s sign was negative. (Plenies´s symptom: percussion tenderness of the right hypogastrium. Blumberg´ s sign: tenderness following the releasing of palpation. Rowsing ´s sign – tenderness in ileocecal region-elicited by palpation of the left hypogastrium after releasing of the pressure against abdominal wall).
His body temperature was 37°C, his pulse rate was 90 beats/minute and his blood pressure was 130/80 mmHg.
The urine examination result was normal.
Laboratory investigations, including serum electrolyte levels and complete blood count, were within normal limits, except for a moderately elevated white cell count (14,000/mm3). A shift of leukocytes to the left side (Neu < 75 %) occurred, too. CRP was elevated: 20 mg/dl.
Imaging methods:
The ultrasound study showed a small amount of free fl uid in the right lower quadrant and tenderness over a non-compressible structure over the iliac vessels, suggestive but not conclusive of acute appendicitis (Fig. 1).
Plain chest and abdominal radiography showed no abnormal signs.
Therapy:
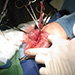
Laparotomy revealed a small amount of clear fluid localized in the right lower quadrant of the abdomen and inflammation at the base of the apendix (Fig 2, 3). Each appendix has its own mesoappendix and its own blood supply derived from appendicular arteries, from the ileocolic artery. Appendix was mobilized, appendiceal artery was ligated and the appendiceal stumps were managed with ligations and inversions using purse strings. Meckel‘s diverticulum was found during inspection of the ileum, and resection with stapler was performed (Fig. 4).
The operative findings correlated with the histopathological finding. Pathology reported the specimen as consistent with early acute appendicitis. Microscopic examination of apendix revealed presence of neutrophils in the gland creating a cryptal abscess - black arrow (Fig. 5).
A drain was placed into the Douglas space.
Postoperatively the patient did well, drain was removed on day four after operation and was released on postoperative day six.
Discussion:
Reginald Fitz first described acute appendicitis in 1886. Until that time the symptoms and pathology of this acute abdominal pain were attributed to typhlitis. Fitz deduced that the most common cause of right lower quadrant pain had it´s origin in the appendix and not in the cecum as was assumed until that time.
Despite appendicitis being the most common reason of acute abdominal pain, its accurate diagnosis remains difficult. Initial symptoms are unspecific and can mimic other diseases, such as gynecological conditions. Female patients of reproductive age were a high-risk group for misdiagnosis.
The diagnosis of appendicitis is primarily based on the patient’s history, physical and laboratory examinations, and imaging techniques such as ultrasonography because they are easily accessable in most hospitals.
The classic epigastric pain that migrates to the right lower quadrant, followed by the onset of subfebrility and vomiting, is present in approximately 40% of patients with appendicitis.
Physical examination is first performed in the ambulance. Mantrels scoring, established by created by Alvarado A. in 1986, is the most famous and the most frequently used point system for clinical and laboratory diagnosis of acute appendicitis. Mantrels score (MS) was used for the evaluation of clinical findings. The points system assesses symptoms and inflammatory markers in a laboratory screening. One point is given to the migration of pain to the right hypogastrium, anorexia, nausea/vomiting, Rovsing’s sign, subfebrility, and shift of the leukocytes to the left side. Two points are given to tenderness in the right lower quadrant and to leukocytosis. Total point count is 10. Patients were divided into four groups according the points scored: Group I: appendicitis was less likely (0-4 points), Group II: possible appendicitis (5-6 points), Group III: probable appendicitis (7-8 points), and Group IV: highly probable appendicitis (>8 points).
Among the laboratory tests, leukocyte count, the shift of leukocytes to the left side and CRP level are the most common inflammatory markers. Serum levels increase at 6-12 hours from initial tissue inflammation. Leukocyte count elevates earlier compare to CRP.
In 1986, Puylaert described an ultrasonographic technique for the diagnosis of acute appendicitis. The sensitivity ranges from 71.3 and specificity from 82. Diagnosis of appendicitis according to ultrasound can be false positive or false negative (visualization is limited by retrocoecal position and presence of gass in caecum), clinical examination, laboratory screening is more important for decision of right diagnosis.
Definitive operative management is open or laparoscopic. In the case of subacute appendicitis, only a drainage of abcessus collection is recommended and removing of apendix is done after resorption of inflamation.
A Meckel diverticulum is a vestigial remnant of the omphalomesenteric (vitellointestinal) duct. As a congenital anomaly, it is a true diverticulum that includes all three coats of the small intestine. Generally, a Meckel diverticulum ranges from 1 to 12 cm in length and is found 45-90 cm proximal to the ileocecal valve. It frequently contains heterotopic tissue, when it does, gastric mucosa accounts for 50%.
Although most commonly discovered as an incidental finding on laparotomy or laparoscopy, Meckel diverticulum can be associated with life-threatening disease states.
Complications manifest as the following: ulceration, hemorrhage, diverticulitisor perforation.
A diagnosis of symptomatic or complicated Meckel diverticulum is difficult to confirm on the basis of traditional history, physical examination, and laboratory testing. It is always considered as a differential diagnosis in cases of intestinal obstruction and intestinal hemorrhage.
Laparoscopy and laparotomy are the most frequent means by which an incidental diverticulum is found.
When a Meckel diverticulum is incidentally discovered at laparoscopy or laparotomy, the surgeon must decide whether to resect. Most surgeons generally do not resect a diverticulum with a wide mouth. However, a diverticulum with a narrow neck, which may obstruct or twist, can be easily resected at the neck without the need for segmental resection. A diverticulum deemed abnormal because of inflammation, thickening, or intramural pathology should be resected, with the decision for local or segmental resection based on the pathology. Removal of a healthy diverticulum in the presence of peritonitis, Crohn disease, ulcerative colitis, or any other complication that would militate against resection is not advised.
Authors declare the case report will not be published in any national or international publications.
Classification ICD-10:
K35 Acute appendicitis, Q43.0 Meckel's diverticulum
4-D assessment:
Textbooks and manuals |
Educational websites and atlases |
Digital video |
Presentations and animations |
Casuistics in images |
E-learning courses (LMS) |
Unreviewed |
Undergraduate level |
Graduate |
Advanced Graduated |
Complex |
HodnoceníPlease select achieved education degree and then evaluate the teaching material particularly in light of material suitability for self-learning.
Student – student of bachelor or master degree
Graduate – graduate of bachelor or master degree PhD. Graduate – Ph.D. student, Ph.D. graduate, researcher, ...
%
Evaluate evaluatethis contribution first! |
Courses
- x [CH-F-E]
- x [CH-F]
- Surgery [ChK/CH-SS-V/17]
- Surgery [1.ChK/CH-SS-ZL/16]
- Surgery 1 [ChK/CH-V1/16]
- Surgery 1 [ChK/CH-ZL1/16]
- Surgery 2 [ChK/CH-V2/09]
- Surgery 2 [ChK/CH-ZL2/15]
- Surgery 3 [ChK/CH-V3/17]
- Surgery 3 [ChK/CH-ZL3/15]
- Surgery 4 [ChK/CH-ZL4/15]
- Surgery 5 [ChK/CH-ZL5/15]
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Martina Vidová Uğurbaş, Lucia Sukovská Lakyová: Appendicitis acuta and Meckel diverticulum. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 27. 05. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=286. ISSN 1337-7000.