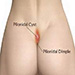
A pilonidal sinus is a sinus track which commonly contains hair. It occurs under the skin between the buttocks at a short distance above the anus. Most cases occur in young male adults. The most commonly used therapy is surgery including incisions, marsupialization, primary midline closure and skin flaps. We present two cases treated with different surgical techniques.
Are the case reports useful for you? Would you also require case reports from other clinical disciplines? Do you have any comments or suggestions for improvement? Please provide your feedback by filling out a short questionnaire.
:: Case report 1
Anamnesis:
A 30 year old male patient came to the surgery with complaints of recurrent discharge from an skin opening in the middle of buttocks with pain, discomfort last three weeks. He had fever last three days. Local finding showed a redness between buttocks, pus discharging through an opening in the skin and painful induration of surrounding tissue.
Therapy:
Acute pilonidal abscess was treated by simple incision in local anaesthesia, surgeon evacuated pus, took a sample of pus to microbiology for cultivation, and gave a drainage with Betadine inside the opened wound. An antibiotic coverage for two weeks was prescribed, and every second day patient visited surgery for dressing of opened wound. Secernation from the wound stopped after four days and wound was healed by secondary intention after two weeks.
A definitive treatment for the pilonidal pit as the underlying cause of the pilonidal disease was necessary as soon as the oedema subsides.
Patient was in need of wide excision after few months because of the risk of recurrence (Figure 1).
Surgeon injected dye into the follicle opening, because it is important to find all the tracks. Patient underwent excision of the diseased tissue down to the sacral fascia and primary closure (Figure 2, 3, 4).
Antibiotic prophylaxis was used before surgery and after surgery for two next days.
The patient was discharged on the three day after the procedure. Sutures are removed on the postoperative fourteen day (Figure 5).
:: Case report 2
Anamnesis:
24 - year- old man was referred to the surgery due to chronic pain between the buttocks , and secernation of clear fluid from fistula. He reported a past history of pharmacological treatment of epilepsy, he didn´t underwent any surgery before.
He complained about inflammation and secretion of yellow, dense fluid, which suddenly disappeared after two weeks 5 months ago. From this incident he suffered from chronic pain and occasionally he had secretion from small opening in the skin. He didn´t have fever.
Therapy:
Because of more fistulas with openings far away from each other, surgeon decided about more radical surgery in comparison to previous case- Limberg flap.
The Limberg flap is a series of communicating equilateral triangles. It is suitable only for closure of rhomboid defects. Before surgery, surgeon draws on the skin around laesion rhombus, which involves affected tissue. After instillation of methylen blue inside fistula, surgeon provides excision and carefully removes all dyed tissue – rhombus of tissue involving pilonidal cyst with all fistulas.
All angles are 60°, which means that every side of both the defect and the flap is equal in length. This orientation creates a flap that is the same size as the defect to be excised. Any flap angle other than 60° theoretically involves either widening or compression of the flap. To address flap survival of the presented technique, the subdermal plexus is considered the source of blood supply to the skin. This network of arterial and venous channels is oriented parallel and adjacent to the skin surface.
An elliptical defect at the donor site remains after the flap is rotated to fill the rhomboid defect. This defect can be closed primarily with appropriate undermining of the surrounding tissue. Extensive mobilization of subcutaneous tissue is necessary. This increases the incidence of postoperative seroma or haemotoma formation. This is reason, why we use closed suction drainage for the patients treated with skin flaps.
Patient received intravenous antibiotics, anti-inflammatory drugs and pain killers after surgery to promote healing, reduce pain and inflammation.
Patient was asked to attend surgical clinic for dressing on alternate days after dismission from hospital in the third postoperative day.
The tracks cut through and simultaneously healed by 2 weeks.
:: Discussion:
The term ‘pilonidal’ was first associated with this condition by Hodges in 1880. It comes from the Latin pilus meaning ‘hair’ and nidus meaning ‘nest’. This term was used to describe the situation of trapped hair in this unusual form of chronic natal cleft skin infection involving skin and subcutaneous tissue.
The sinus track goes in a vertical direction between the buttocks.
It is most likely that sacrococcygeal pilonidal infection originates within a natal cleft hair follicle, which becomes distended with keratin. The distended follicle becomes inflamed and the resulting folliculitis produces oedema, which blocks the follicle opening. The obstructed follicle then expands and finally ruptures into the underlying subcutaneous fat to form a pilonidal abscess. In addition, hair is a secondary invader, being drawn into the abscess cavity by the suction effect along the gluteal cleft that results from the movement of the buttock.
The disease was described as jeep disease, becauses drivers of jeeps, who are fatty, hairy, sweating with low hygiene suffer often from this disease.
There are different methods in the surgical treatment of pilonidal disease: marsupialization, primary midline closure and skin flaps.
The success of the excision and primary closure is directly related to the complete excision of the sinus cavity and the tracks.
Closing the defect by avoiding dead space underneath is necessary.
Excision and skin flaps seem to be more successful in large pilonidal disease and recurrent cases although the hospital stay is longer. But in uncomplicated cases, excision and primary closure gives better results. This minimally invasive procedure minimizes rates of complication and recurrence and enables the patient to as early as possible. Risk of recurrence is higher in the case of smaller excision compare to wide excision and using of flap, but complications (infection, haematoma, dehiscence of suture) after wider excision and creating of flap are worse.
The average healing time after operation is 14 days.
Wound infections, wound breakdowns, collections of seroma or haematoma, and recurrence are common complications after procedure.
Recurrences after treatment of pilonidal disease are usually observed within the first 3 years.
Early recurrences after treatment are usually associated with wound infection and incomplete excision of pilonidal disease.
To identify the sinus and all of the tracks and therefore, to lower the recurrences, injection of methylene blue into the opening is very helpful.
Authors declare the case report will not be published in any national or international publications.
Classification ICD-10:
sinus pilonidalis, surgical treatment
4-D assessment:
Textbooks and manuals |
Educational websites and atlases |
Digital video |
Presentations and animations |
Casuistics in images |
E-learning courses (LMS) |
Unreviewed |
Undergraduate level |
Graduate |
Advanced Graduated |
Complex |
HodnoceníPlease select achieved education degree and then evaluate the teaching material particularly in light of material suitability for self-learning.
Student – student of bachelor or master degree
Graduate – graduate of bachelor or master degree PhD. Graduate – Ph.D. student, Ph.D. graduate, researcher, ...
%
Evaluate evaluatethis contribution first! |
Courses
- x [CH-F-E]
- x [CH-F]
- Surgery [ChK/CH-SS-V/17]
- Surgery [1.ChK/CH-SS-ZL/16]
- Surgery 1 [ChK/CH-V1/16]
- Surgery 2 [ChK/CH-V2/09]
- Surgery 3 [ChK/CH-V3/17]
- Surgery 5 (Neurosurgery, Orthopedics) [ChK/CH-V5/09]
- Surgery 1 [ChK/CH-ZL1/16]
- Surgery 2 [ChK/CH-ZL2/15]
- Surgery 3 [ChK/CH-ZL3/15]
 Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
Contribution content is subject to licence Creative Commons Uveďte autora-Neužívejte dílo komerčně-Nezasahujte do díla Attribution 3.0 Czech Republic
citation: Martina Vidová Uğurbaş, Lucia Sukovská Lakyová: Management of pilonidal sinus. Multimedia support in the education of clinical and health care disciplines :: Portal of Pavol Jozef Šafárik University in Košice Faculty of Medicine [online] , [cit. 05. 04. 2026]. Available from WWW: https://portal.lf.upjs.sk/articles.php?aid=276. ISSN 1337-7000.